If you have spent months researching the precision of bone-shaving techniques for your facial feminization, you have likely focused on the CT scans of your mandible. However, the most successful V-line outcomes are not dictated by the bone alone, but by how the soft tissue reacts to the sudden lack of skeletal support. Without mentalis muscle suspension, even the most perfect surgical cut can result in a sagging, distorted lower face known as the ‘witch’s chin.’ This guide explores the mechanical necessity of muscle reattachment during genioplasty to ensure your functional recovery and aesthetic harmony remain intact.
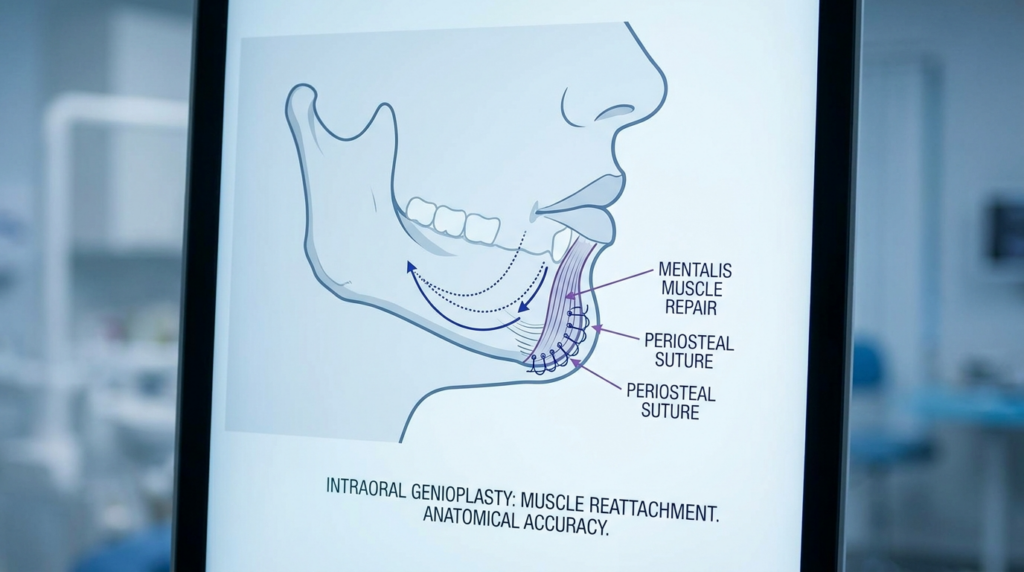
Table of Contents
Mentalis Muscle Suspension: The Structural Bridge Between Bone and Beauty
The mentalis muscle is the primary elevator of the lower lip and the soft tissue of the chin. Unlike many other muscles that connect bone to bone, the mentalis originates from the symphyseal bone (the front of your chin) and inserts directly into the skin. This unique anatomy creates a “mousetrap” effect: once the muscle is detached from the bone during an intraoral incision, it naturally wants to snap downward and backward. If a surgeon performs a chin contouring (genioplasty/mentoplasty) without a deliberate plan for mentalis muscle suspension, the result is soft tissue ptosis.
Specifically, when we talk about ptosis in the lower face, we are describing a condition where the chin pad hangs lower than the bone. This creates a redundant fold of skin that obscures the sharp jawline you just paid for. Therefore, understanding the suspension process is not just about avoiding a complication; it is about ensuring that your new, smaller chin actually looks like a natural part of your face. Consequently, the surgical focus must shift from what is being removed (the bone) to what is being preserved (the muscle-to-skin tension).
Why Symphyseal Bone Exposure Demands Precise Reattachment
During a V-line or genioplasty procedure, the surgeon must strip the periosteum and the mentalis muscle away from the bone to access the mandibular symphysis. This symphyseal bone exposure is a surgical necessity, but it leaves the muscle “homeless.” Without a stable anchor point to return to, the muscle fibers contract and heal in a lower position. This creates a deepening of the labial sulcus—the space between your lower lip and your gums—which can lead to food trapping and speech impediments. Specifically, the loss of muscle tension makes it difficult to fully close the mouth, a condition known as lip incompetence.
Moreover, the aesthetic price of ignoring mentalis muscle suspension is high. When the muscle sags, the lower lip often turns outward (ectropion) or drops down, exposing more of the lower teeth even when at rest. This gives the face an aged, “toothy” appearance that contradicts the goals of facial feminization surgery. Therefore, the reattachment technique must be robust enough to withstand the constant movement of the mouth during talking and eating throughout the healing phase.
The Comparison: Reattachment vs. Neglect
| Feature | With Proper Suspension | Without Proper Suspension |
|---|---|---|
| Chin Pad Position | Firmly anchored to the new bone contour | Sagging below the bone (Ptosis) |
| Lower Lip Function | Full elevation and competence | Lip drop, lower tooth exposure |
| Labial Sulcus Depth | Maintained at natural levels | Abnormally deep or shallow |
| Smile Dynamics | Natural, symmetrical muscle pull | Asymmetrical or “stiff” smile |

Preventing Soft Tissue Ptosis: The Intraoral Incision Paradox
Most V-line surgeries utilize an intraoral incision to avoid external scarring. While this is great for hiding scars, it makes mentalis muscle suspension more challenging. Because the incision is inside the mouth, gravity is constantly pulling the detached muscle downward. Surgeons must use specialized muscle reattachment techniques to pull the mentalis back up and secure it to the periosteum or, in some cases, directly to the bone using drill holes and non-resorbable sutures. Specifically, this “pull-up” technique ensures the chin pad follows the new, smaller skeletal framework rather than collapsing under its own weight.
In addition to the physical reattachment, the depth of the initial incision plays a massive role. If the incision is too high, there isn’t enough muscle left to grab and pull. If it’s too low, the labial sulcus is destroyed. For instance, at the Feminization Center, our approach involves a mid-level incision that leaves a “cuff” of tissue on the bone side. This cuff acts as a reinforced anchor point for the suspension sutures, significantly reducing the risk of soft tissue sagging during the critical first six weeks of healing.
The Science of Labial Sulcus Depth and Functional Recovery
Functional recovery after jaw surgery is often measured by how quickly you can eat or speak, but the true measure is the restoration of the labial sulcus. This groove is essential for speech articulation and oral hygiene. When mentalis muscle suspension is performed incorrectly, the sulcus can become “obliterated,” meaning the muscle heals directly to the gum line. This prevents the lower lip from moving independently of the chin pad. Consequently, patients often describe a “wooden” feeling in their lower face that never truly goes away.
To prevent this, surgeons must focus on intraoral incision healing that respects the three-dimensional space of the sulcus. Using “double-layer” suturing—where the muscle is closed first and the mucosa (inner mouth lining) is closed second—is vital. This prevents the muscle from sliding down the bone. Furthermore, using a chin strap or compression garment post-operatively isn’t just for swelling; it provides the external support needed to keep the muscle pressed against the bone while the internal sutures do their work.

Muscle Reattachment Techniques: From Periosteal to Transosseous
There are two primary schools of thought regarding mentalis muscle suspension. The first is periosteal suturing, where the muscle is stitched back to the thick layer of tissue covering the bone. This is effective for standard genioplasty where bone reduction is moderate. However, in aggressive V-line cases or significant chin reductions, there may not be enough periosteum left to hold the weight of the muscle. In these scenarios, transosseous (through the bone) suspension is the gold standard. The surgeon drills tiny holes in the mandible to loop sutures directly through the bone, creating an unbreakable bond.
Particularly in jaw reduction (reshaping or tapering), the loss of surface area on the bone means the muscle has less “real estate” to stick to. Therefore, transosseous suspension becomes the primary insurance policy against the “witch’s chin.” While it takes longer to perform, the long-term benefit of a stable, youthful chin position far outweighs the extra 20 minutes in the operating room. This level of detail is what separates a standard cosmetic result from a high-precision feminization outcome.
Intraoral Incision Healing: What Patients Must Monitor
Your role in preventing muscle ptosis doesn’t end when the anesthesia wears off. The way you care for your mouth during the first month determines whether the mentalis muscle suspension holds. Specifically, you must avoid pulling your lower lip down to “check the stitches.” This repetitive tension can cheese-wire the sutures through the delicate muscle tissue, causing the suspension to fail. Furthermore, a diet of soft foods is not just about your teeth; it’s about minimizing the forceful contraction of the mentalis muscle while it is trying to fuse to the bone.
Watch for signs of “dimpling” or a “deepened crease” below the lower lip. While some swelling is expected, a permanent horizontal groove often indicates that the muscle has slipped. If you notice your lower lip is resting lower than usual, exposing your bottom teeth, it is crucial to contact your surgical team immediately. Early intervention with specialized taping or even minor resuturing can often save the aesthetic result before the tissue becomes permanently scarred in a dropped position.
The Step-by-Step Protocol for Soft Tissue Preservation
Achieving a flawless lower face contour requires a disciplined approach from both the surgeon and the patient. This protocol outlines how to ensure your mentalis muscle suspension is successful and your recovery is optimized for the best possible aesthetic outcome.
- Verify the Technique: During your consultation, specifically ask your surgeon how they plan to reattach the mentalis muscle. Ensure they are familiar with transosseous suspension if you are undergoing significant bone reduction.
- Prioritize Periosteal Integrity: A skilled surgeon will preserve as much periosteum as possible during the symphyseal bone exposure to provide a strong base for reattachment.
- Execute Multi-Layer Closure: Ensure the surgical plan includes a dedicated layer of sutures for the muscle itself, independent of the mucosal closure.
- Commit to External Compression: Wear your chin compression garment religiously for the first 2 weeks. This eliminates the “dead space” between the muscle and bone, allowing them to fuse properly.
- Limit Mimetic Movement: Avoid excessive talking, laughing, or wide yawning for the first 14 days. Every time you move your chin, you are testing the strength of the suspension sutures.
- Monitor the Labial Sulcus: Keep the incision site clean with salt-water rinses to prevent infection, which is the leading cause of suture breakdown and muscle slippage.
- Schedule Functional Checks: At your 1-month and 3-month follow-ups, have your surgeon evaluate your lip competence and smile symmetry to ensure the muscle is healing in the correct anatomical position.
By following these steps, you transition from a passive patient to an active participant in your recovery. Remember, the bone provides the shape, but the muscle provides the life. Protecting the mentalis muscle suspension is the only way to ensure your new jawline is as functional as it is beautiful.

Common Questions Regarding Chin Muscle Reattachment
What exactly happens if mentalis muscle suspension is not performed?
If the mentalis muscle is not properly suspended, it sags due to gravity and natural contraction. This results in ‘witch’s chin’ deformity, where the soft tissue of the chin pad hangs below the bone. This not only looks aged but also causes functional issues like lip incompetence and difficulty speaking or keeping the mouth closed naturally.
How long do the suspension sutures need to hold the muscle?
The internal sutures typically need to provide maximum support for 4 to 6 weeks. During this window, the mentalis muscle undergoes biological fusion with the underlying bone or periosteum. Once this biological bond is strong enough, the sutures are no longer the primary support. This is why following post-op restrictions during the first month is so critical for a permanent result.
Can a sagging chin be fixed after it has already healed?
Yes, but a secondary mentalis muscle suspension is more complex than the primary one. It involves reopening the intraoral incision, removing scar tissue, and lifting the muscle back to its original position. Because the muscle may have shortened or become fibrotic, results are more predictable when the suspension is done correctly during the initial V-line or genioplasty surgery.
Will I feel the sutures used for the muscle suspension?
Most patients do not feel the internal sutures, as they are buried deep within the muscle and tissue layers. Surgeons often use dissolvable sutures that last several weeks, or tiny non-resorbable ones that are well-tolerated by the body. You might feel a sensation of tightness in the chin for a few months, which is a sign that the suspension is maintaining the necessary tension.

