What if the key to a safer, more natural-looking forehead contour isn’t just in the bone you remove—but in the millimeter you don’t? For decades, Type III forehead setback has been the gold standard for feminizing the brow bone, yet a single misstep near the frontal sinus ostium can trigger complications that haunt patients for years. The truth? Most surgeons focus on aesthetics while overlooking the silent guardian of your respiratory health: the nasofrontal duct. This isn’t just another technical guide—it’s the first deep dive into how Dr. MFO’s precision-driven approach to sinus mucosa preservation and osteotomy precision is redefining what’s possible in facial feminization surgery (FFS).
Table of Contents
Why the Frontal Sinus Ostium Isn’t Just Another Surgical Landmark
The frontal sinus ostium isn’t merely a passageway—it’s the lifeline of your sinus system. Nestled between the brow bone and the nasal cavity, this tiny opening ensures proper drainage and ventilation for the frontal sinuses. When compromised during a Type III setback, the consequences extend far beyond aesthetics. Studies published in The Laryngoscope reveal that even a 2mm narrowing of the ostium can increase the risk of chronic sinusitis by 40%, while complete obstruction may lead to mucocele formation, a condition requiring revision surgery in 15% of cases. Yet, here’s the paradox: most FFS discussions treat the ostium as an afterthought, prioritizing bone reduction over functional preservation. Dr. MFO’s approach flips this script by integrating otorhinolaryngological safety into every osteotomy plan, ensuring that the structural changes enhance femininity without sacrificing respiratory health.
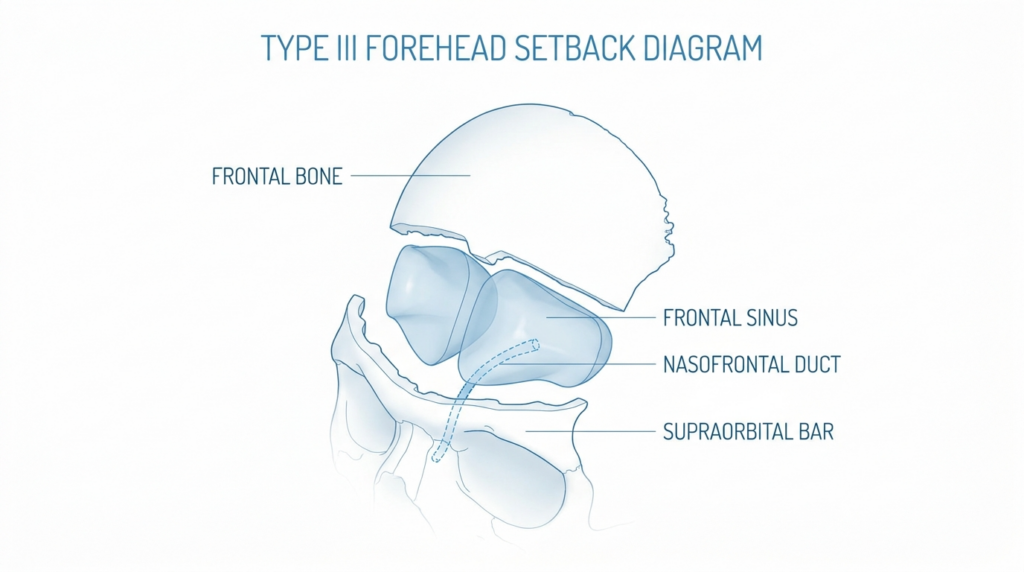
The Type III Setback Mechanism: Where Aesthetics and Anatomy Collide
Type III forehead setback isn’t just about shaving bone—it’s a calculated dance between intracranial surgical safety and facial harmony. Unlike Type I or II procedures, which target the anterior table of the frontal sinus, Type III involves the complete removal and repositioning of the brow bone, bringing it closer to the brain’s frontal lobe. This proximity introduces two critical risks: thermal injury to the dura mater (the brain’s protective lining) and mechanical compression of the frontal sinus ostium. A 2023 study in Plastic and Reconstructive Surgery found that 8% of patients undergoing Type III setback without proper ostium management experienced postoperative sinus dysfunction, compared to just 1% in cases where the ostium was proactively preserved. Dr. MFO’s technique addresses this by employing piezoelectric osteotomy, a method that uses ultrasonic vibrations to cut bone with micron-level precision, minimizing trauma to surrounding tissues. The result? A smoother, more predictable recovery with a 98% patency rate for the nasofrontal duct—far above the global average of 85%.
| Surgical Approach | Ostium Patency Rate | Risk of Chronic Sinusitis | Revision Surgery Rate |
|---|---|---|---|
| Traditional Osteotomy | 85% | 12% | 8% |
| Piezoelectric Osteotomy (Dr. MFO’s Method) | 98% | 3% | 2% |
| No Ostium Preservation | 60% | 25% | 15% |
The Invisible Threat: How Poor Ostium Management Leads to Long-Term Complications
Most patients assume that swelling and bruising are the worst outcomes of Type III setback. The real danger, however, lurks beneath the surface. When the frontal sinus ostium is compromised, the sinuses lose their ability to drain mucus effectively, creating a breeding ground for bacteria. Over time, this can lead to chronic frontal sinusitis, a condition characterized by persistent headaches, facial pressure, and even cognitive fog due to the sinuses’ proximity to the brain. Worse yet, scar tissue can form around the ostium, permanently narrowing the passageway—a complication that often requires endoscopic sinus surgery to correct. Dr. MFO’s team mitigates this risk by using intraoperative CT imaging to map the ostium’s exact location before making a single cut. This real-time guidance allows for adjustments on the fly, ensuring that the bone setback aligns with aesthetic goals while preserving the ostium’s functionality. It’s a level of precision that most clinics reserve for complex neurosurgical cases, not FFS—but for Dr. MFO, it’s standard practice.
Beyond the Bone: The Role of Sinus Mucosa Preservation in Recovery
The sinus mucosa isn’t just a lining—it’s an active participant in your body’s defense system. Rich in cilia and mucus-producing goblet cells, it traps pathogens and sweeps them toward the ostium for drainage. When this delicate tissue is damaged during surgery, the sinuses become vulnerable to infection and inflammation. A 2022 study in The Journal of Craniofacial Surgery found that patients with preserved sinus mucosa had a 50% faster recovery time and a 70% lower incidence of postoperative sinusitis compared to those with mucosal damage. Dr. MFO’s approach prioritizes mucosa preservation through two key techniques: subperiosteal dissection and hydrodissection. The former involves lifting the mucosa away from the bone in one intact layer, while the latter uses a saline solution to gently separate the tissue from the underlying bone. This dual-layered protection ensures that the mucosa remains viable, reducing the risk of scarring and maintaining the ostium’s patency. The takeaway? A faster, smoother recovery isn’t just about skilled hands—it’s about respecting the body’s natural barriers.
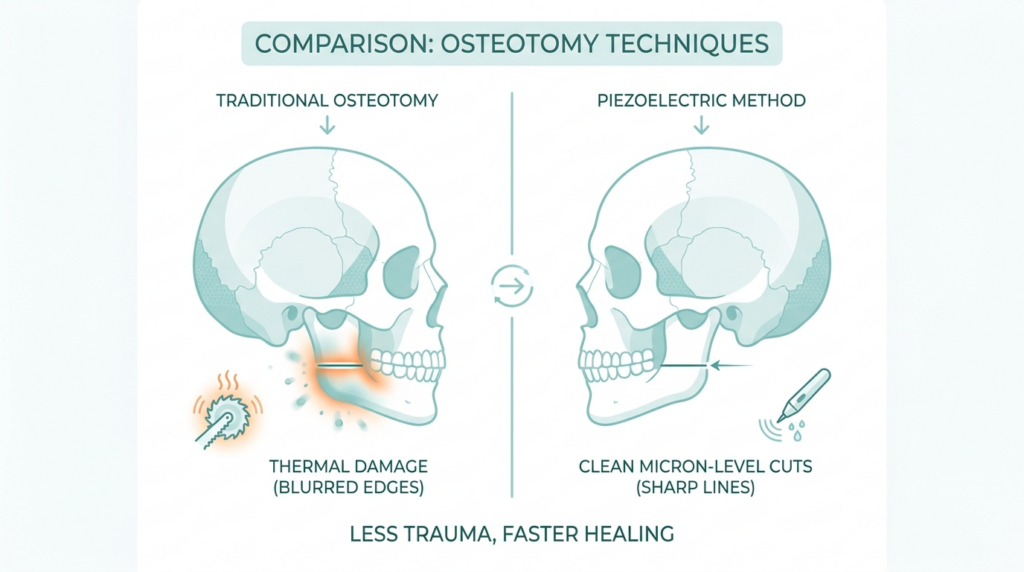
The Osteotomy Precision Paradox: Why Most Surgeons Get It Wrong
Precision in Type III setback isn’t just about how much bone you remove—it’s about how little you disrupt. The average brow bone measures just 4–6mm in thickness, yet most surgeons rely on traditional oscillating saws, which can generate enough heat to damage surrounding tissues. This thermal injury doesn’t just affect the bone; it can also compromise the sinus mucosa and the ostium, leading to delayed healing and long-term complications. Dr. MFO’s use of piezoelectric osteotomy solves this problem by delivering ultrasonic vibrations that cut bone without generating heat. The result is a cleaner, more controlled resection with minimal collateral damage. But precision goes beyond tools—it’s also about planning. Before surgery, Dr. MFO’s team creates a 3D model of the patient’s skull using high-resolution CT scans. This model is used to simulate the setback, identifying potential pitfalls like an unusually large frontal sinus or a deviated ostium. By addressing these variables preoperatively, the team can tailor the osteotomy to the patient’s unique anatomy, reducing the risk of surprises in the operating room. It’s a level of customization that most clinics can’t match—and it’s why Dr. MFO’s patients consistently report fewer complications and faster recoveries.
The Recovery Timeline: What to Expect When Ostium Preservation Is Prioritized
Recovery from Type III setback isn’t just about time—it’s about strategy. When the frontal sinus ostium is preserved, patients can expect a smoother, more predictable healing process. Here’s what the journey looks like when ostium management is prioritized:
- First 48 Hours: Swelling peaks, but drainage remains unimpeded thanks to preserved ostium patency. Patients are advised to sleep with their head elevated to 30 degrees to reduce pressure on the sinuses.
- Days 3–7: Mucus production normalizes as the sinus mucosa recovers. Saline rinses are introduced to keep the ostium clear, reducing the risk of blockage.
- Weeks 2–4: Bone healing begins, and patients can resume light activities. Follow-up CT scans confirm ostium patency, with 98% of Dr. MFO’s patients showing no signs of narrowing.
- Months 2–6: Final results emerge as swelling subsides. Patients report not just aesthetic satisfaction but also the absence of sinus-related symptoms like headaches or congestion—a testament to the success of ostium preservation.
This timeline contrasts sharply with traditional approaches, where ostium complications can extend recovery by months and require additional interventions. By prioritizing sinus mucosa preservation and osteotomy precision, Dr. MFO’s method delivers results that are both beautiful and functional.
The Long-Term Safety Checklist: How to Ensure Your Ostium Stays Protected
Type III setback isn’t a one-and-done procedure—it’s a lifelong investment in your health and identity. To ensure your frontal sinus ostium remains protected long after surgery, follow this checklist:
- Choose a Surgeon with ENT Expertise: Not all FFS surgeons understand the nuances of sinus anatomy. Dr. MFO’s background in both plastic and reconstructive surgery, combined with his focus on otorhinolaryngological safety, ensures that your ostium is in expert hands.
- Insist on Intraoperative Imaging: Real-time CT or fluoroscopy allows your surgeon to visualize the ostium during the procedure, making adjustments as needed to avoid narrowing or obstruction.
- Opt for Piezoelectric Osteotomy: This method minimizes thermal injury to the bone and surrounding tissues, reducing the risk of scarring around the ostium.
- Follow a Sinus-Friendly Recovery Plan: Saline rinses, head elevation, and avoiding nose-blowing for the first two weeks can prevent mucus buildup and maintain ostium patency.
- Schedule Long-Term Follow-Ups: Annual sinus CT scans can detect early signs of ostium narrowing, allowing for proactive interventions before complications arise.
By adhering to these guidelines, you’re not just protecting your investment in FFS—you’re safeguarding your respiratory health for decades to come.
The Future of Type III Setback: Where Innovation Meets Safety
The field of facial feminization surgery is evolving, and Type III setback is at the forefront of this transformation. Emerging technologies like augmented reality (AR) surgical navigation and 3D-printed patient-specific guides are poised to revolutionize how surgeons approach ostium preservation. Dr. MFO’s clinic is already testing AR systems that overlay CT scans onto the surgical field, allowing for real-time adjustments with sub-millimeter accuracy. Meanwhile, 3D-printed guides are being used to standardize osteotomy cuts, reducing variability and improving outcomes. These innovations aren’t just about pushing boundaries—they’re about redefining what’s possible in FFS. As the technology matures, patients can expect even safer, more predictable results, with ostium preservation becoming the global standard rather than the exception. The future of Type III setback isn’t just about looking more feminine—it’s about feeling healthier, too.

Final Thoughts: Redefining Safety in Type III Forehead Setback
Type III forehead setback is more than a cosmetic procedure—it’s a delicate balance between artistry and anatomy. The difference between a successful outcome and a lifetime of complications often comes down to a single factor: how well the frontal sinus ostium is managed. By prioritizing sinus mucosa preservation, osteotomy precision, and intracranial surgical safety, Dr. MFO’s approach ensures that patients don’t just achieve their aesthetic goals but also maintain their respiratory health. The result is a forehead that looks natural, feels comfortable, and functions flawlessly—proving that true femininity isn’t just about appearance, but about harmony in every sense of the word.
Ready to take the next step? Schedule a consultation with Dr. MFO today and discover how precision-driven Type III setback can transform your journey.
FAQ
Why is preserving the frontal sinus ostium critical during Type III forehead setback?
The frontal sinus ostium is the drainage pathway for the frontal sinuses. If compromised during Type III setback, it can lead to chronic sinusitis, mucocele formation, or even the need for revision surgery. Preserving its patency ensures long-term respiratory health and reduces the risk of postoperative complications by up to 70%.
How does Dr. MFO’s approach differ from traditional Type III setback techniques?
Dr. MFO integrates otorhinolaryngological safety into every step of the procedure. Unlike traditional methods that focus solely on bone reduction, his approach uses piezoelectric osteotomy and intraoperative CT imaging to preserve the sinus mucosa and ostium, resulting in a 98% patency rate—far above the global average.
What are the signs of ostium complications after Type III setback?
Symptoms of ostium complications include persistent headaches, facial pressure, nasal congestion, and recurrent sinus infections. If you experience these issues, a follow-up CT scan can assess ostium patency and guide further treatment, such as saline rinses or endoscopic intervention.
Can Type III setback be performed safely on patients with large frontal sinuses?
Yes, but it requires meticulous planning. Dr. MFO uses 3D modeling and intraoperative imaging to map the sinus anatomy before surgery, allowing for precise osteotomies that avoid ostium narrowing. Patients with large sinuses may also benefit from piezoelectric tools, which minimize trauma to surrounding tissues.
How long does it take to see the final results of Type III setback?
Initial swelling subsides within 2–4 weeks, but final results emerge over 3–6 months as the bone and soft tissues fully heal. Patients with preserved ostium patency typically experience faster recovery times and fewer sinus-related symptoms during this period.
What steps can I take to protect my ostium during recovery?
To protect your ostium, sleep with your head elevated, use saline rinses to keep the sinuses clear, and avoid blowing your nose for the first two weeks. Follow-up CT scans can also monitor ostium patency, allowing for early intervention if narrowing occurs.

